Our optometrists strive to stay current with the latest diagnostic tools and treatments in order to provide the best eye care to the Pembina Valley. Utilizing the latest optometry technology allows our optometrists to diagnose diseases at the earliest stages possible when they are most easily managed and treated.
EYE HEALTH INSTRUMENTATION
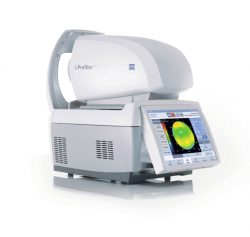
With this digital technology your prescription can be measured to 1/100th of a dioptre, offering crisper, brighter vision, especially at night. The iProfiler Plus takes into account your unique “eye print” (corneal map) which enables your optometrist to prescribe the most precise, balanced prescription for you. The corneal map or topography is a three-dimensional image of the surface of the cornea, the clear tissue at the front of the eye. Having this information is helpful in diagnosing corneal diseases such as Keratoconus earlier.
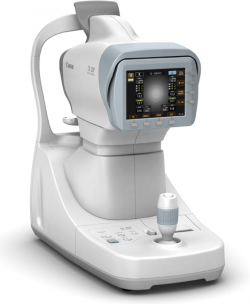
There are 2 separate components to this automated optical equipment.
The first component is the auto refraction. Auto refraction is a computer determined measurement of a person’s prescription. The prescription is not exact, but gives the doctor good baseline information or a starting point of the subjective refraction. It is of particular benefit when dealing with non-communicative people such as young children or those with disabilities.
Auto refraction is a relatively quick and simple procedure. The patient sits behind the instrument and places their chin on the chin rest. They simply need to look into the instrument at a picture, which may go in and out of focus. On an average person, the test takes 10-15 seconds to perform and no feedback is required by the patient.
The second component is the auto keratometer. Auto keratometry is a computer determined measurement of the curvature of the central cornea or shape of the front surface of the eye. It is used in optometric practice for contact lens fitting, detection of certain diseases (keratoconus) and as a component of determining laser eye surgery candidacy. The procedure is identical to that of auto refraction. In fact, the instrument does both of these measurements simultaneously.

Measuring and verifying the prescription of your current eyewear is important to ensure that they are exactly as ordered and to monitor prescription changes. The Lensometer is also used to measure how well your current sunwear are blocking ultraviolet light.

Non-Contact Tonometer (NCT):
This instrument measures the internal pressure of your eyes known as the Intraocular Pressure (IOP). Pachymetry, a measurement of your corneal thickness, can be obtained at the same time on our instrument. This measurement is required to ensure that the pressure readings are within range for your given eye anatomy. IOP measurements are an important part of identifying inflammation and glaucoma risk. This test is particularly important because you have no internal sensation to tell you if your eye pressure is abnormal.
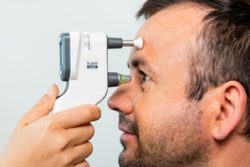
iCare Tonometer:
This “puff-less” instrument also measures your internal eye pressure (IOP). It measures your IOP without the puff of air, as with the non-contact tonometer. You can request this test over the “puff of air” test if you prefer.
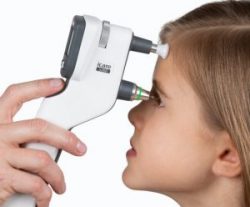
The FDT measures your central and side vision using a variety of light patterns. It has been instrumental in detecting early eye disease and neurological (brain) disease.
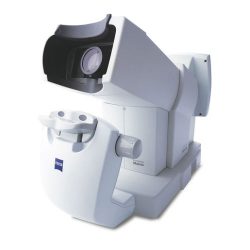
Optomap California Retinal Imaging
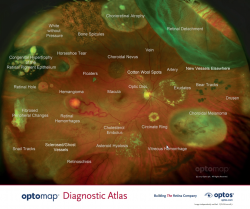
The Optomap non-invasively captures an instantaneous, ultra-widefield digital scan of the retina, revealing important information for the comprehensive evaluation of systemic and ocular health. Using the 200⁰ image of the back of your eye, the retina, your optometrist is easily able to detect any abnormalities. It also takes a scan using autofluorescence. Fundus autofluorescence or FAF imaging gives information over and above conventional imaging techniques such as fundus retinal photos as it allows visualization of retinal metabolic changes and helps to identify areas that may be at high risk for certain eye diseases. Optomap and FAF have been so integral to the diagnosis of eye pathology, Focal Point has made it a standard of care in our practice.
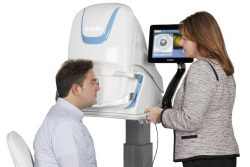
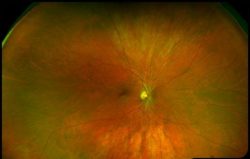
Optomap Monaco Retinal Imaging
The Optomap non-invasively captures an instantaneous, ultra-widefield digital scan of the retina, revealing important information for the comprehensive evaluation of systemic and ocular health. Using the 200⁰ image of the back of your eye, the retina, your optometrist is easily able to detect any abnormalities. It also takes a scan using autoflourescence. Fundus autoflourescence or FAF imaging gives information over and above conventional imaging techniques such as fundus photos as it allows visualization of retinal metabolic changes and helps to identify areas that may be at high risk for certain eye diseases. Optomap and FAF has been so integral to the diagnosis of eye pathology, Carman Vision Services has made it a standard of care in our practice. The Monaco combines Optomap ultra-widefield technology with OCT creating a fast, convenient, multi-modal imaging tool. It can produce a 200°, single-capture retinal images of unrivaled clarity and can display a six-image overview including color, Autofluorescence (AF), and OCT of both eyes in as little as 90 seconds.
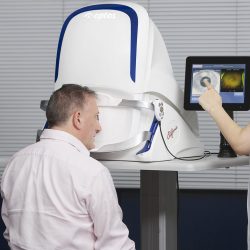
Optomap Monaco OCT Imaging
Using OCT technology your optometrist will be able to see a detailed view of your macula. It will help detect retinal diseases such as macular degeneration much earlier. This exciting technology is part of your routine adult and senior eye exam.
This non-invasive infrared camera images the meibomian glands. Meibomian glands sit within your eyelids and produce oils which form the outermost, or top, layer of your tears. Damage to, or loss of, these glands can lead to dry eye disease.
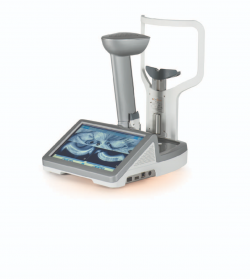
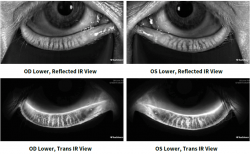
The microscope in the optometrist’s office is an instrument that is used to assess the external and internal structures of your eyes.

“Which is better 1 or 2?” Through a series of questions and processes your optometrist will use your feedback and the collected data to calculate the most precise and balanced prescription to ensure you are seeing your best.

SPECIALIZED TECHNOLOGY
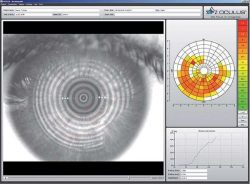
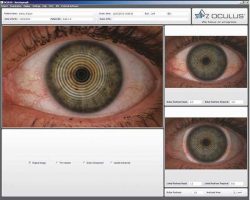
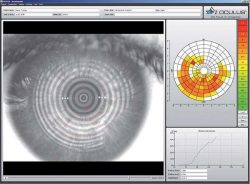
The OCULUS Keratograph 5M is an advanced corneal topographer with built in colour camera for imaging the front surface of the eye. In patients with Dry Eye Disease (DED) we use this instrument to image the meibomian (oil) glands in the eyelids, the lipid layer of the tears and how quickly the tears dry on the surface of the eye.
As a topographer the OCULUS provides detailed corneal mapping over a wide area of the cornea. This information allows our doctors to assess corneal pathologies and provide accurate contact lens fittings.


Systane® iLux 2® is a handheld device that is designed to heat and apply gentle pressure on the eyelids to open up blocked meibomian glands (the oil glands). This makes it easier for the glands to naturally release their oil which is so important for a good quality tear film. The device has a specially designed eyelid smart tip that gently delivers treatment directly to the blocked glands while protecting the surface of the eye. Your ocular hygienist has complete control with iLUX® and administers the therapeutic effect.
The treatment takes approximately 8-12 minutes for both eyes. The therapeutic light-based heat will begin to warm the blocked glands to a safe temperature to soften and release the oil. With gentle pressure and heat, the oil will be expressed from the glands and the treatment is complete.
Intense pulsed light (IPL) is a standard treatment for skin rosacea that is also effective for treating dry eye. High-intensity light energy warms the oil in the meibomian glands, allowing them to be expressed and improve their function. IPL shrinks inflamed blood vessels, reduces inflammatory chemical factors on the eye and tear film, and is effective against Demodex. IPL can also provide collagen tightening and some aesthetic improvement to the skin around the eyes.
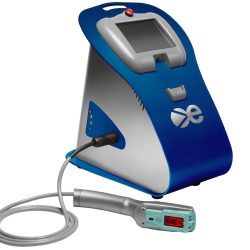
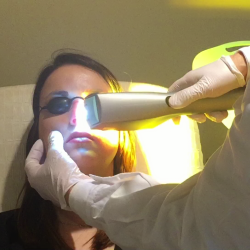
Low-level light therapy (LLLT) utilizes long-wavelength red LED light to stimulate the meibomian glands on both the upper and lower eyelids.


BlephEx is an in-office medical device used in the fields of ophthalmology and optometry to treat blepharitis and dry eye disease. The handheld device is used by your eye doctor to exfoliate the eyelid at the lash line and remove the inflammatory biofilm that leads to chronic lid disease and discomfort.


The TearLab Osmolarity System* is intended to measure the osmolarity of our patients to aid in the diagnosis of dry eye disease (DED) in patients suspected of having dry eye disease, in conjunction with other methods of clinical evaluation. Test results help your optometrist determine the right treatment plan for you.

The OCT scan is a painless way to diagnose eye diseases that tend to progress without any symptoms in the early stages – eye diseases that could lead to irreversible blindness.
The OCT uses laser light to produce a highly detailed cross-section of the various tissues inside the eye, much like an ultrasound. Your optometrist can see the surface layers when they look inside your eye; the OCT shows them the layers underneath. It allows for detection of very subtle changes that may affect your eye health but are not measured using traditional methods. The OCT is part of our standard of care to detect and manage glaucoma, macular degeneration, complications caused by diabetes and retinal damage due to certain medications. Pachymetry (thickness of the cornea) measurements can also be obtained with this instrument.

OCT Angiography (OCT A)
AngioPlex® OCT Angiography from ZEISS ushers in a new era of eye care with non-invasive imaging of retinal blood vessels – taking glaucoma and retinal disease management and treatment planning to the next level. Imaging the retinal vascular system in great detail will allow us to detect various diseases such as macular degeneration, diabetic retinopathy, vascular occlusions, earlier.
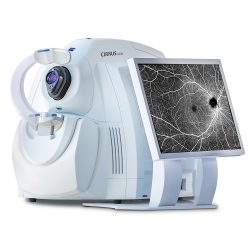
Anterior Segment OCT
Anterior segment OCT is taking ultrasound images of the front of the eye including the cornea, anterior chamber, drainage angle, and lens. It provides comprehensive imaging and quantification of the anterior segment for refractive surgery planning and follow-up, corneal evaluation, and glaucoma risk assessment. It can also be used to help fit and assess specialty rigid contact lenses.
Similar to, but more detailed than the FDT, the HFA uses a series of hundreds of flashing lights at different intensities to quantify small defects of your central and side vision. Subtle weaknesses are not always visible to you and can appear in a visual field test result before any visual loss is noticed. These tests are essential in monitoring the health of the eye after surgery or changes due to glaucoma and neurological disorders, such as strokes and brain tumors. The HFA is also used in vision assessments for drivers’ licenses and determining eligibility for eyelid surgery covered by Manitoba Health.
The Zeiss IOL (Intra Ocular Lens) Master allows fast, accurate measurements of eye length and surface curvature. These readings are necessary in measuring the progression of myopia. It can also be used to determine the power of the Intraocular lens used in cataract and lens implantation surgery.

FRAME AND LENS MEASUREMENTS
In today’s on-the-move, always connected world, you have the freedom to browse, double-tap, zoom, or pedal… whenever and wherever you want. Multitasking is now a part of everyday life, so you need a lens solution that can keep up with your connected lifestyle. Today’s sophisticated, modern lenses depend on the accuracy of their fitting. In fact, a lens can lose up to 40% of its optical performance due to inaccurate centration.
The i.Terminal 2 quickly and comfortably captures and calculates precise measurements (within 0.1mm) that are required for all FreeForm (high-definition) lenses.

ZEISS’ i.Terminal Mobile allows us to take fast, accurate measurements in a convenient and flexible manner for our diverse and valued patient base.