Frequently Asked Questions
General
As a general guideline, our Optometrists support the following recommendations of the Canadian Association of Optometrists:
Infants/Toddlers (0-4 years) First exam between 6-12months of age
Exam at age 3
Exam prior to school entry
School age (5-18 years) Exam annually
Adults (19-64) Exam every 1-2 years
Seniors (65 years and older) Exam every 1-2 years
Cost of an Eye Exam in Manitoba
The services provided in a comprehensive eye exam require time, staff, equipment, technology, and ongoing training. Optometrists set their professional fees based on a number of factors and there may be variation in fees charged due to the equipment used, the fee structure in place, and other factors.
Manitoba Health insures basic optometric eye exams for children 0-18 years old every year and seniors aged 65+ every 2 calendar years. Ocular health exams for Manitobans of any age with diagnosed eye disease or those defined as high risk for developing eye disease (ex. If you have diabetes) are also insured. Ask your optometrist if you are eligible for insured benefits. If you are eligible for an insured eye exam, your optometrist will be able to bill some services to Manitoba Health on your behalf.
Manitoba Health does not insure all services or tests required to diagnose, follow, and treat certain eye diseases. These additional charges are the patient’s responsibility. Your optometrist or the staff will advise you of the fees and charges for services to be performed prior to the provision of services. If you have extended health insurance, ask your plan administrator what is covered under your vision benefit. Although Manitoba Health does not insure corrective or therapeutic services (eyeglasses, contact lenses, visual training), some private insurance group health plans will cover a portion of these costs.
A Doctor of Optometry (O.D.) is a provincially licensed health care provider specifically educated and clinically trained to examine the eyes and the visual system. Optometrists detect, diagnose and treat vision problems.
Optometrists work in collaboration with family practitioners and ophthalmologists (medical/surgical eye specialists) to ensure that patients receive a level of care required by their particular eye or general health concerns.
Common Vision Concerns
Nystagmus is an involuntary rhythmic side-to-side, up and down or circular motion of the eyes that occurs with a variety of conditions.
Amblyopia, or lazy eye, is the loss or lack of development of vision in an eye that is healthy. Amblyopia can be caused by crossed-eyes (strabismus), unequal refractive error, farsightedness or nearsightedness, or a physical obstruction like a cataract. The brain “learns” to see with the good eye only, and the other eye grows weaker from disuse. It is estimated that 2 – 4% of all children have amblyopia. Amblyopia is responsible for more cases of vision loss in children than all other ocular diseases and traumas combined. If detected and treated at an early age, amblyopia will often resolve completely.
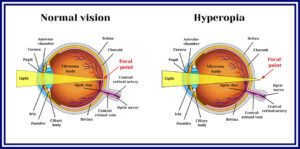
Hyperopia (Far-sightedness)
Hyperopia is a common vision condition in which you can see distant objects clearly, but objects nearby may be blurry. The degree of your farsightedness influences your focusing ability.
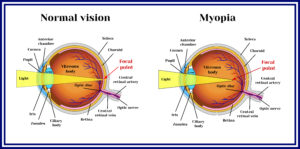
Myopia (Near-sightedness)
Myopia is a common vision condition in which you can see objects near to you clearly, but objects farther away are blurry. It occurs when the shape of your eye causes light rays to bend (refract) incorrectly, focusing images in front of your retina instead of on your retina.
Myopia Management
Most myopia is caused by the eye length growing too quickly in childhood. The eyes are meant to grow from birth until the early teens and then cease, but in myopia the eyes grow too much and/or continue growing into the teenage years. Excessive eye growth raises concern because even small amounts of stretching can lead to increased likelihood of vision threatening eye diseases in later life, such as myopic macular degeneration, retinal detachment, glaucoma, and cataract.
Myopia management aims to apply specific treatments to slow excessive eye growth to a lesser rate. Experts agree that myopia management should be commenced for all children under age 12, and typically continue into the late teens.
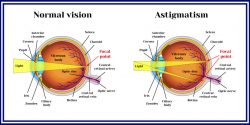
Astigmatism means “without a single focal point”. Typically the curves of the front of the eye (the cornea) focus light on the retina. In patients with astigmatism no sharp focus occurs. Astigmatism can often be corrected with glasses, contacts or refractive surgery.
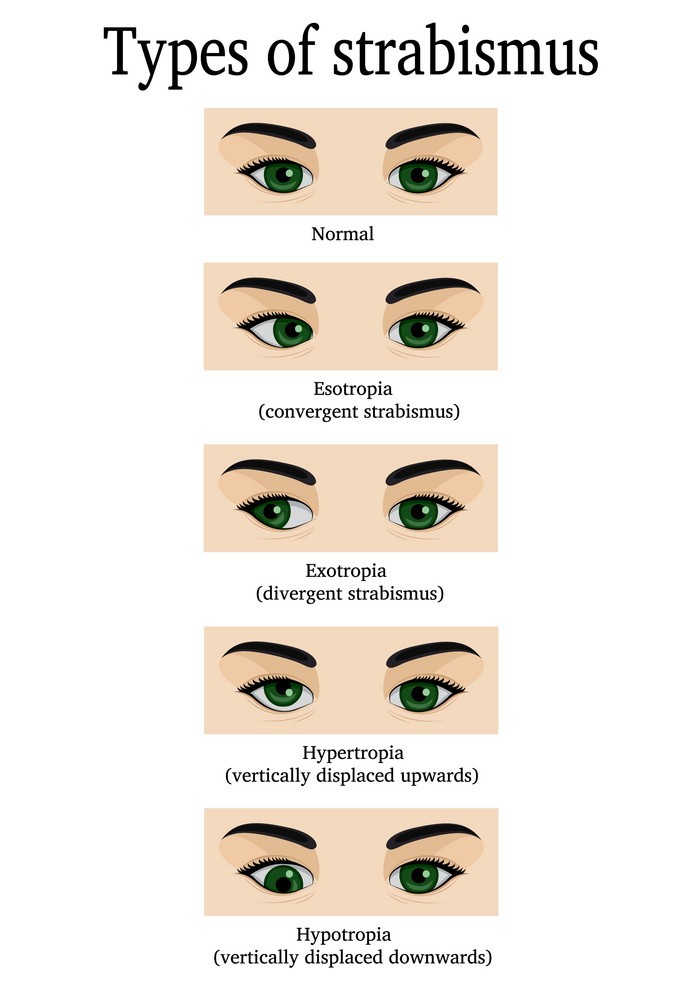
Strabismus is the abnormal alignment of the eyes. This occurs when the eye muscles point one or both eyes in the wrong direction. The brain will have difficulty in blending the two images, problems with depth perception and double vision may occur. Treatment for strabismus may include glasses, prisms, vision therapy and in some cases, surgery.
Floaters are tiny clumps of gel or cells inside the vitreous, the clear jelly-like fluid that fills the inside of your eye. You may sometimes see small specks or clouds moving in your field of vision. They are more noticeable when looking at a plain background, like a blank wall or blue sky.
While some floaters may remain in your vision, many of them will fade over time and become less bothersome. Moving your eyes can help to move the floaters out of the way. There is currently no treatment for floaters.
Floaters can be a symptom of a retinal tear or detachment. A prompt retinal exam is required with an appearance of any new floaters.

Right now there is limited scientific evidence to suggest that screens are permanently damaging the eyes but research is ongoing.
We do know that extended screen use results in a reduced frequency of blinking. This can lead to significant dry eye disease if not properly managed or treated.
You may notice increased eye strain, fatigue or discomfort with extended viewing of screens. It is always advisable to first have a complete eye examination to rule out eye disease and provide proper glasses, if you need them.
It has also been proven that blue light emitted from screens can disrupt your sleep-wake cycle. Many lenses can now be ordered with blue light filters, like ZEISS BlueGuard or ZEISS DuraVision BlueProtect, to reduce your exposure to blue light with extended screen use.
Some helpful hints to try and reduce symptoms include: taking breaks from screen time, lubricating eye drops and ensuring the screen is positioned below eye level. With the increasing availability of eye drops be sure to ask your optometrist what they would recommend for your use.
Eye Health Concerns
A cataract is a clouding or fogging of the normally clear and transparent lens inside the eye. Light cannot be properly focused on the retina resulting in an unclear image.

The normal process of aging can cause the lens to harden and turn cloudy resulting in senile cataracts. These are the most common type and may occur as early as age 40.
Eye injuries can cause cataracts in people of any age. A hard blow, puncture, intense heat or chemical burn can potentially damage the lens, resulting in a traumatic cataract.
Certain systemic diseases, such as diabetes mellitus, may also cause the lens to cloud resulting in secondary cataracts.
Infrequently cataracts may develop in children. Certain infections affecting the pregnant mother may cause cataracts to develop in the unborn baby. Alternatively they can be hereditary in nature.
Depending on the size and location of the cloudy areas in the lens, a person may or may not be aware that a cataract is developing. As cataracts develop there may be hazy, fuzzy, blurred or double vision. The eyes tend to become more sensitive to light and glare, making night driving difficult.
A routine ocular health exam can diagnose cataracts. Your optometrist may need to dilate your pupils to properly assess the severity of the cataract.
Sometimes a stronger glasses prescription can help to provide clarity as a cataract develops. When a cataract causes loss of sight that interferes with your work or lifestyle, it probably is time to have it removed. Surgery is the only effective way to remove the cloudy lens.
Cataract surgery is performed by Ophthalmologists and is highly successful. During this procedure the cloudy lens is removed and a replacement lens is implanted inside the eye. This lens is called an intraocular lens (IOL). This replacement restores one’s sight to pre-cataract conditions. It is important to note that, as with all surgeries, results cannot be guaranteed and if other ocular health conditions exist vision may not be perfect after surgery.
Reduce your exposure to ultraviolet radiation (UV) over your lifetime. It is very important to wear sunglasses to protect your eyes that have 100% UV protection. In addition to sunglasses, a wide brimmed hat will help protect your eyes.
Cigarette smoke is known to contain substances that interfere with the eye’s antioxidant defense mechanisms, increasing the risk of developing cataracts.
More than 1 alcoholic drink per day increases the risk of cataracts. Scientists believe that alcohol in the body is converted into a harmful substance called acetaldehyde that may damage the eye’s lens.
Researchers are seeking ways to boost the eye’s natural ability to fight UV. Nutrients called antioxidants (such as Vitamins A, C, and E, beta-carotene and lutein) found in some fruits and vegetables may help the lens to protect itself against UV radiation. Research is not yet clear on whether supplementing your regular diet with these nutrients can lower your risk of cataract, but studies continue.
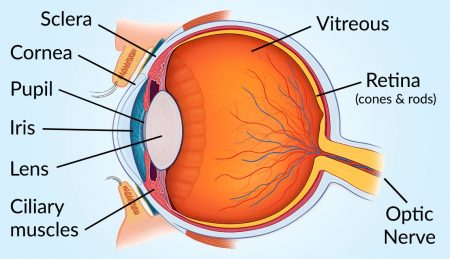
Cornea – clear front surface of the eye
Pupil – the aperture or window allowing light into the eye
Crystalline lens (lens) – helps focus light on the retina.
Retina – is the innermost layer of the back of the eye. Formed of light sensitive nerve endings that carry visual information to the optic nerve.
Macula – a small area in the retina that provides our most central, acute vision. (Example: Driving, reading, etc.)
Choroid – consists of blood vessels and is the inner coat between the sclera and retina.
Sclera – the white of the eye. Provides the structural shape of the eye.
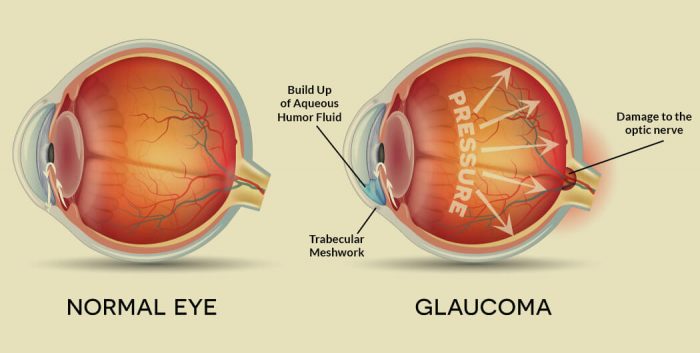
Glaucoma is a group of diseases where the optic nerve is damaged causing a loss of peripheral, or side, vision. This damage can be related to the eyes intraocular pressure (IOP). If glaucoma goes undetected or untreated it can cause damage to the optic nerve resulting in a loss of vision and even blindness. Glaucoma is the second leading cause of blindness in Canada.
A clear fluid called the aqueous humor nourishes the lens, cornea and iris. This fluid is continually produced and drained where it is absorbed back into the bloodstream. If a block in drainage occurs, or excess fluid is produced, eye pressure may be increased. Normal pressure is considered to be between 10 and 21 mmHg.
Although glaucoma can occur at any age, it is more common as people age. Other risk factors include persons with diabetes, vascular disorders and a family history of glaucoma. As with any disease early detection is important.
Glaucoma cannot be prevented, but it can be treated. Our Optometrists monitor the optic nerve for changes at every eye exam and start monitoring intraocular pressure at age 13.
With the use of prescription eye drops and in some cases laser treatments and/or surgery to lower the pressure inside the eye, glaucoma can be treated. Frequent reviews of peripheral vision (visual field testing), intraocular pressure and the structure of the optic nerve are important to ensure glaucoma is well controlled. Typically patients with glaucoma will be followed with an appointment every 6 months. Our optometrists are trained and licensed to treat open angle glaucoma with topical eye drops. We are fortunate to be able to co-manage many other cases with our ophthalmologists in Winnipeg.
Macular degeneration (AMD) is an eye disease that affects central vision. This is the area responsible for fine details such as sewing, reading and face recognition. Even in its most severe form, a person with AMD will still have good peripheral vision, however, the ability to see details will be lost.

There are two forms of macular degeneration:
Dry: A slow breakdown or death of light sensing cells in the retina. This results in a gradual loss of central vision. Most macular degeneration is dry.
Wet: A less common form in which abnormal, new blood vessels grow beneath/into the retina. The abnormal blood vessels leak and bleed resulting in sudden and severe loss of central vision. Wet ARMD patients can have rapid progression in as little as days to months.
Eye Care Products and Services
If your optometrist recommends that you fill a prescription for corrective lenses, you probably will consider the purchase of glasses. This involves frame and lens selection, as well as prescription verification and fitting the glasses to your face for comfort.
More than fashion must be considered when selecting glasses. Your specific vision needs may not be suited to a particular type of lens or frame. The prescription itself, as well as, the intended use for the glasses (e.g. work, recreation or other lifestyle factors) are considerations to take into account. Other important choices involve the right lens type, such as bifocal or progressive, glass or plastic, and whether high index (thinner) lenses should be considered. This is critical in achieving satisfaction in the performance of your glasses.
Even with these particular considerations in mind, the choice today in both frames and lenses is vast. Our opticians can help you select a frame that is well made, the right size, comfortable, attractive, and within your budget.
Contact lenses are advantageous over glasses in that they allow a natural field of view since there are no frames to obstruct side vision, and the wearer usually looks through the center of the lens where the vision is the best. However, they are medical devices, in that they rest on the eye, and regular eye health monitoring is essential for safe, long term use of contact lenses.
In order to determine a prescription for contact lenses, supplemental ocular health assessments must be made by the prescribing doctor to ascertain whether your eyes can safely accept contact lenses and, if so, the appropriate parameters for those lenses. These additional tests, evaluation and diagnosis are not considered part of a routine eye examination.
Contact lens technology has come a long way in the last few years. New materials, designs, and manufacturing techniques have resulted in contact lenses that provide visual correction for almost any eye condition. These include farsightedness, nearsightedness, astigmatism and presbyopia. So, if you were ever told you couldn’t wear contact lenses, it’s time to ask again.
The cost of contact lenses varies according to an individual’s prescription. Our contact lens fees are part of a comprehensive fitting program to provide you with convenient, carefree and safe contact lens wear. Our licensed contact lens technician will be happy to explain the program most suitable to your visual needs.
Yes. We have a free “try-on” contact lens visit available for any individual who is interested in contact lenses. This free trial also includes trying on tinted contact lenses.
